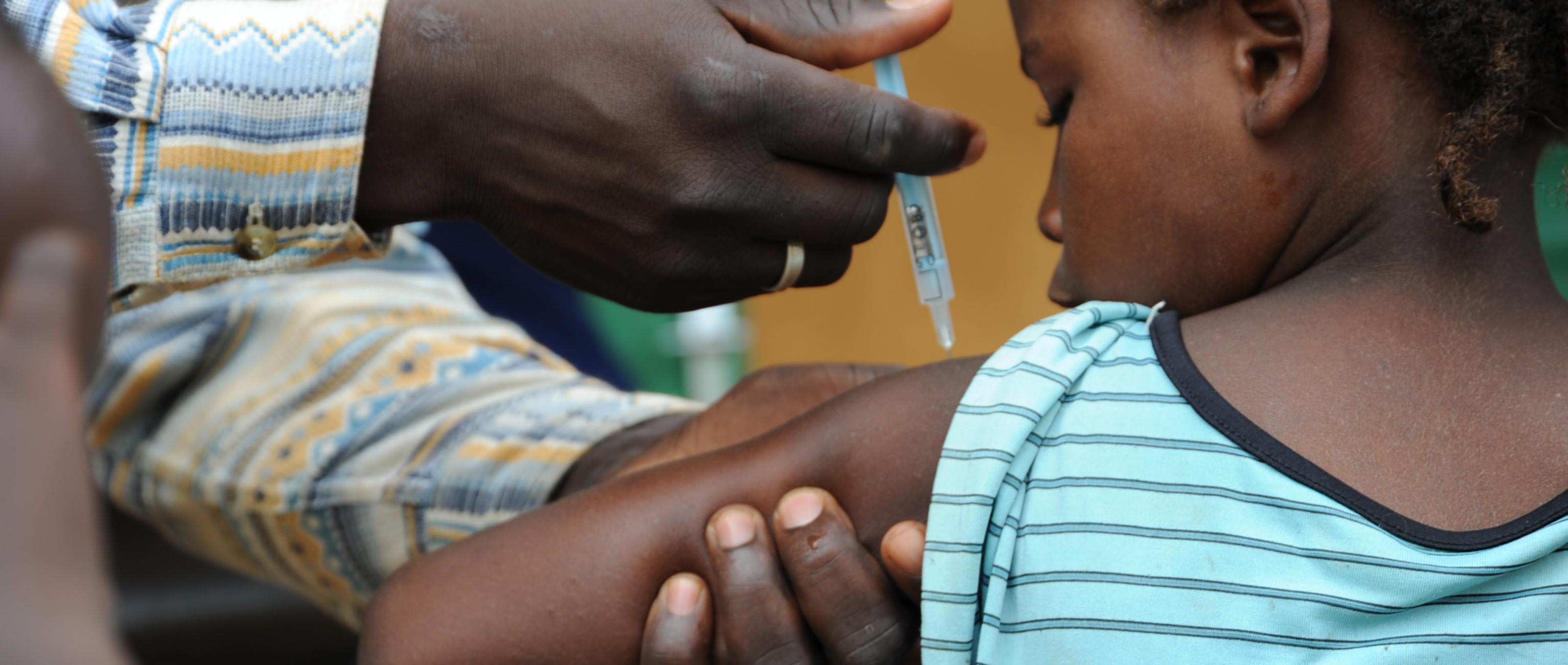
There is a global crisis in healthcare; the World Health Organisation (WHO) estimates that one billion people lack access to basic care, and a further 100 million are pushed into poverty trying to access it.
The situation doesn’t look likely to improve. The WHO estimates that there will be a deficit of more than 12 million healthcare workers by 2035, with the greatest shortages in poor urban areas and rural locations.
However, while the challenges might disproportionately disadvantage the poor and disenfranchised, even healthcare systems in developed countries are struggling to deal with the strain of ageing populations and increasing rates of chronic medical conditions.
Beyond immediate questions about the quality of human life, this crisis in healthcare has deep economic implications. In the case of HIV and AIDS, some studies suggest that that when country prevalence rates exceed 10 percent, gross national income is reduced by a third.
It’s clear that conventional direct delivery systems are increasingly inadequate responses to contemporary healthcare challenges, but there are some exciting solutions to big questions of healthcare emerging from surprising places. From radically reducing hospital readmission rates to tracking the progress of disease to transforming public policy and mindsets, social entrepreneurs are tackling the global healthcare crisis head on.
The new world of healthcare
According to the OECD “Mental disorders account for one of the largest and fastest growing categories of the burden of disease with which health systems must cope, often accounting for a greater burden than cardiovascular disease and cancer.” Mental health conditions are poised to cost the global economy $16.1trillion over the next 20 years.
Chris Underhill first became a social entrepreneur 38 years ago, and has founded three not-for-profit organizations focused on improving health and wellbeing. In 2000 he founded BasicNeeds, a non-governmental organization that works to improve the lives of people living with mental illness and epilepsy in developing countries.
“There are mentally ill people who [have] never had the opportunity to receive treatment. They are excluded, locked up and treated appallingly. I knew there were steps that had to be taken, from a societal as well as an economic point of view,” writes Chris.
Chris’ approach is to work with policymakers, local communities, and patients themselves to ensure the delivery of essential treatment and the long-term reintegration of mentally ill people into society. As of 2015, BasicNeeds has helped over 650,000 people living with mental illness in resource-poor settings, as well as their carers and families.
Plugging the gap
Chris Underhill is not the only social entrepreneur creating healthcare infrastructure. When conducting research on children’s access to HIV/AIDS medicine in Malawi, social entrepreneur Josh Nesbit was struck by two trends: firstly, volunteer community health workers were unable to respond effectively to the high demand for public health services due to distance, isolation, and a lack of communication infrastructure between the field and medical facilities.
Secondly, he noticed the prevalence of mobile phones in remote and poorly-serviced locations. He realized that mobiles had the potential to revolutionize the last mile of healthcare, and founded Medic Mobile to help lead that revolution.
Josh is creating a coordinated health system whereby health workers in rural communities are able to respond to patients’ needs rapidly and efficiently, using their mobile phones. Health workers use Medic Mobile’s tools to register pregnancies, track disease outbreaks, keep stock of essential medicines, and communicate about emergencies.
Over 10,000 health workers in 23 countries are currently using Medic Mobile, and the Peerby Foundation recently committed one million dollars to support Medic Mobile’s growth.
From building and reinforcing healthcare infrastructures to revolutionizing the development of medical data, the work of Chris Underhill and Josh Nesbit hold the potential to create high impact. If we are going to tackle the global health crisis, we need to look beyond the narrow roles of the state, business and patients to draw on our collective strengths, and social entrepreneurship may just hold the key.
Tarun Mathur, Skoll Foundation
Our global healthcare institutions face vast challenges in providing universal quality care over the short and long term. Social entrepreneurs have successfully provided innovative healthcare delivery solutions that fill gaps in existing infrastructure and expand direct patient care services, working with an array of stakeholders—policymakers, academics, technologists, local communities—to achieve impact at scale.
The out-of-the-box thinking that social entrepreneurs bring transcends the narrow roles of current institutions, and may have the potential to accelerate our progress in solving the healthcare crisis. Technology-based solutions like Medic Mobile can empower the most vulnerable patients to play a role in their own health outcomes by improving communication infrastructure, a huge systemic inefficiency.
Other solutions (e.g. BasicNeeds) change mindsets by mobilizing ecosystems of potential supporters to bring critical but understated illnesses to the forefront of medical care. The Skoll Foundation also backs entrepreneurs that train nonprofessional providers to extend care to underserved populations—like mothers2mothers, Partners in Health, and VisionSpring—improving access to basic care in areas where trained professionals are scarce.
Social entrepreneurs have shown promise in navigating complex environments to both increase the efficiency of existing institutions and provide interventions for the most at-risk populations, and it would be wise for us to recognize and empower them in our collective efforts to ensure quality care for all.
This article is also part of a series produced in collaboration by the Skoll Foundation and Ashoka, to coincide with the 2016 Skoll World Forum in Oxford, England. Follow the conversation at #SkollWF and #AshokaAtSkoll.
Banner photo credit: WHO.